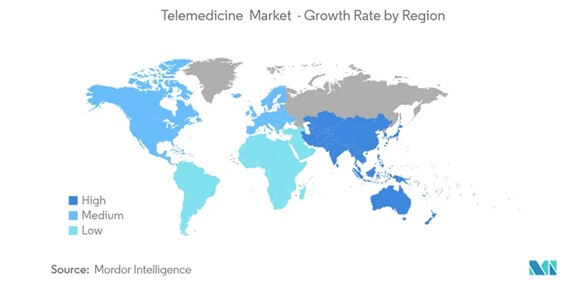
The Growth of the Global Telemedicine Market
Valued at $50 billion in 2019 and with a projected growth potential of $460 billion by 2030, the global telemedicine market is a significant driver of the digital transformation of the healthcare industry. Beyond delivering access to high-quality healthcare services despite geographical barriers and underdeveloped infrastructure, telemedicine is also bringing healthcare delivery costs down significantly, making it a promising endeavor in developing countries. This growth is being further fueled by increased funding for telemedicine, higher costs of accessing traditional or physical healthcare services, and an uptick in digital users.
When was telemedicine introduced?
Broadly speaking, the term ‘telemedicine’ came into use in the 1970s, but no standard definition was adopted until much recently, when the World Health Organization proposed that it is:
The delivery of health care services, where distance is a critical factor, by all healthcare professionals using information and communication technologies for the exchange of valid information for diagnosis, treatment and prevention of disease and injuries, research and evaluation, and for the continuing education of healthcare providers, all in the interests of advancing the health of individuals and their communities.
As such, one of the first times that telemedicine came into play was possibly during the 1860s – with telegraph messages being transferred for the treatment of injured soldiers during the U.S. Civil War. An early 20th century account has also been published, discussing the transmission of ECG data over the telephone. From these early times, with substantial communications in the military, teaching hospitals, television services, and the aviation and space sectors, telemedicine has come a long way to being delivered over cost-effective satellite communications technology.
The benefits of Telemedicine in Developing Countries
In developing countries, concerns such as underdeveloped infrastructure, unreliable electric grids, and spotty internet connections in rural areas make access to healthcare difficult, and frankly impossible, for a huge population. However, with growing access to smartphones and wireless technologies, telemedicine is potentially available at the click of a button. Not only does this address several logistical issues in the delivery of healthcare in developing countries, it expands the scope of access to the global level. The increased use of telemedicine services is tangibly demonstrating a reduced need to travel over long distances to access healthcare, optimised healthcare professionals staffing and associated costs, fewer in-patient stay requirements, and improved management of chronic diseases.
Satcom Technology for Telemedicine
Mobile apps, video calls, and secure data transfers require a reliable communication link and satellite technology is most suitable for optimising such processes for healthcare delivery. From remote monitoring of healthcare resources and decreased time for diagnosis, consultations, results, and reviews to digitalisation of healthcare records, test results, and best practice information and potential standardisation of clinical protocols and medical training, the use of satellite technology allows for reduced costs in overall healthcare delivery.
A 2011 NetMotion Wireless Survey demonstrated how beautifully satellite communications technology bridges the gap between healthcare services available in urban and rural areas. With telemedicine over a wireless network, medical professionals were able to reach out to remote and isolated communities and 63% of respondents shared that wireless data applications helped to increase their productivity levels at mobile clinics that were a part of hospital systems.
Governments in developing countries are increasingly investing in connectivity – at higher and higher speeds – in rural areas. Currently, the demand for mobile health monitoring applications is increasing dramatically. According to WHO, four in five developing countries offer at least one mobile healthcare program for essential healthcare services.
Besides Low Earth Orbit (LEO) satellite services for internet coverage, 5G connectivity is expected to further expand the scope of telemedicine services. From quicker data transfers of high-quality images and videos to VR services, telemedicine is not just about diagnosis anymore. With 5G, it may be possible to conduct surgeries over virtual and digital technology.
Advanced technologies such as the Internet of Things (IoT), artificial intelligence (AI), and algorithms that diagnose rare diseases, cancer, and COVID-19 are serving to increase the investment in digital healthcare services. In 2020, the United Arab Emirates (UAE) put forth a proposal to work with telecom operators to build its first virtual hospital.
The Impact of the COVID-19 Pandemic on the Growth of Telemedicine
The COVID-19 pandemic further accelerated the spread of telemedicine. A McKinsey Report indicates that the use of telemedicine has increased 38 times from the pre-COVID-19 era.
It states that China and India are likely to lead the growth of the digital healthcare market in Asia, valued at a projected US$100 billion by 2025, with Malaysia, Indonesia, Philippines, and Vietnam showing immense potential for telemedicine services. The government in Indonesia encouraged virtual consultations and pharmaceutical delivery networks for mild COVID-19 cases, demonstrating the growing trend towards the digitalisation of healthcare services in ASEAN countries.
Besides alleviating the immense pressure on governments in developing countries to offer access to healthcare services, the benefits of telemedicine services have been made crystal clear to end-users during large-scale lockdown and social distancing measures – and are in demand even in the aftermath of the COVID-19 pandemic.
The COVID-19 pandemic has ushered in a new era of healthcare services delivery, where the spread of diseases has potentially global implications. As such, technological advances in telemedicine are being funded and supported by governments across the world to ensure affordable and innovative solutions.
For example, video calls have become common and their use has been preferred evidently during the COVID-19 pandemic. According to an analysis by Deloitte, this preference for video over non-video methods of communication is rising and has clear implications for telemedicine. On the one hand, it is likely that a permanent shift by end-users to video calls over voice calls and emails can occur in the near future, and on the other hand, video calls can increase the effectiveness of healthcare consultations. Moreover, telemedicine consultations have reduced the physician-patient visit time by 20%, making these a more efficient means of communication.
Portable Telemedicine Kits by IEC Telecom
Satellite communications technology has made it possible to develop telemedicine hubs that offer real-time healthcare consultations in underserved or unserved areas. Moreover, it also supports healthcare providers in the digital or virtual administration of this evolving aspect of healthcare, including appointment scheduling, logistics, accounting, and opportunities to collaborate with other healthcare professionals across the world.
Keeping in mind these specific requirements of the healthcare sector – and in light of the growing demand for telemedicine in a post-COVID-19 era – IEC Telecom offers two powerful telemedicine kits. OneHealth and OneHealth Mini (powered by DigiGone) bring virtual care to patients wherever they are located.
OneHealth has been designed to care for patients who are homebound or live in areas with limited to no primary healthcare availability. It supports the real-time transmission of patient data over an award-winning intuitive software that is housed in a waterproof and rugged case. It empowers the doctor or medical specialist to make informed diagnoses with multi-party video, voice, and text as well as remote control of the camera. OneHealth comes equipped with a Bluetooth thermometer, pulse oximeter, blood pressure monitor, and glucose meter as well as an electronic stethoscope and otoscope to enable the onsite attendant to quickly support the diagnosis process and apply treatment options.
OneHealth Mini has been designed for those on-the-go. It provides secure communications to a medical professional using a Wi-Fi hotspot, cellular or satcom connection. The secure multi-party video calling capability allows multiple medical specialists in different locations to collaborate simultaneously for an efficient diagnosis process. OneHealth Mini comes equipped with a Bluetooth thermometer, pulse oximeter, blood pressure monitor, and glucose meter. Its lightweight, rugged, and simple design makes it a highly portable telemedicine kit at an affordable price for anyone with internet access.
Future Drivers of Telemedicine
Such telemedicine kits, mobile health apps, and active remote monitoring of vital statistics seem to be the logical evolution of telemedicine in developing countries, reflecting both the increased demand from end-users as well as the investment by governments. Undoubtedly, regulation for telemedicine services will need to be standardised and made intrinsic to the delivery essential healthcare. Healthcare providers and patients will both need access to training for effective use of telemedicine services over such digital dashboards and apps. And satellite communications technology will need to incorporate an even stronger process to ensure the security, privacy, and reliability of healthcare information transfers in areas with no/limited GSM coverage.